 
Knowledge from molecular and cell biology, medicine, manufacturing, materials science and nanotechnology must be amalgamated in a multi-disciplinary manner to develop successful periodontal and peri-implant tissue engineering treatment approaches. In order to tackle the complexity of regenerating the periodontium which is composed of numerous cell types and tissue interfaces, therapeutic approaches in TE/RM must draw from many fields of research spanning both the basic science and clinical realms. Some of the major clinical challenges encountered in periodontal tissue engineering and alveolar bone augmentation include developing strategies to overcome masticatory forces, the avascularity of the tooth and implant surfaces, and the microbial contamination inherent to working in the oral cavity. Bone regeneration applies specifically to the treatment of peri-implant hard tissue deficiencies, alveolar ridge defects in need of augmentation for future implant placement and sinus floor augmentation. Periodontal regeneration is an important component of this vast field and involves the reconstitution of cementum, periodontal ligament (PDL) and alveolar bone around teeth. Craniofacial tissue engineering employs a wide range of approaches generally centered on conduction and induction of host cells, as well as cell transplantation and gene therapy. The field of tissue engineering/regenerative medicine (TE/RM) has emerged to manage these clinical scenarios, with the goal of replacing and regenerating lost or damaged tissues to restore normal function and structure. Besides periodontitis and peri-implantitis, orofacial soft and hard tissue deficiencies can also be caused by post-extraction atrophy, trauma, tumor resection, and congenital or developmental conditions such as cleft lip and palate. These microbially-mediated inflammatory diseases are destructive in nature and culminate in progressive loss of tooth-supporting alveolar bone. The management of periodontal and peri-implant diseases constitutes a significant healthcare burden with the potential to greatly improve the quality of life of affected patients. The present narrative review discusses key advancements in PTEBR including current and future trends in preclinical and clinical research, as well as the potential for clinical translatability. Periodontal tissue engineering and bone regeneration (PTEBR) aims to improve the state of patient care by promoting reconstitution of damaged and lost tissues through the use of growth factors and signaling molecules, scaffolds, cells and gene therapy. In many cases, it is still challenging to achieve predictable regenerative outcomes utilizing current approaches. Although these approaches have shown positive outcomes for small and medium-sized defects, predictability of clinical outcomes is heavily dependent on the defect morphology and clinical case selection. Current regenerative approaches utilized in everyday clinical practice are mainly guided tissue/bone regeneration-based. Ultimately, regenerated periodontal and peri-implant support must be able to interface with surrounding host tissues in an integrated manner, withstand biomechanical forces resulting from mastication, and restore normal function and structure. 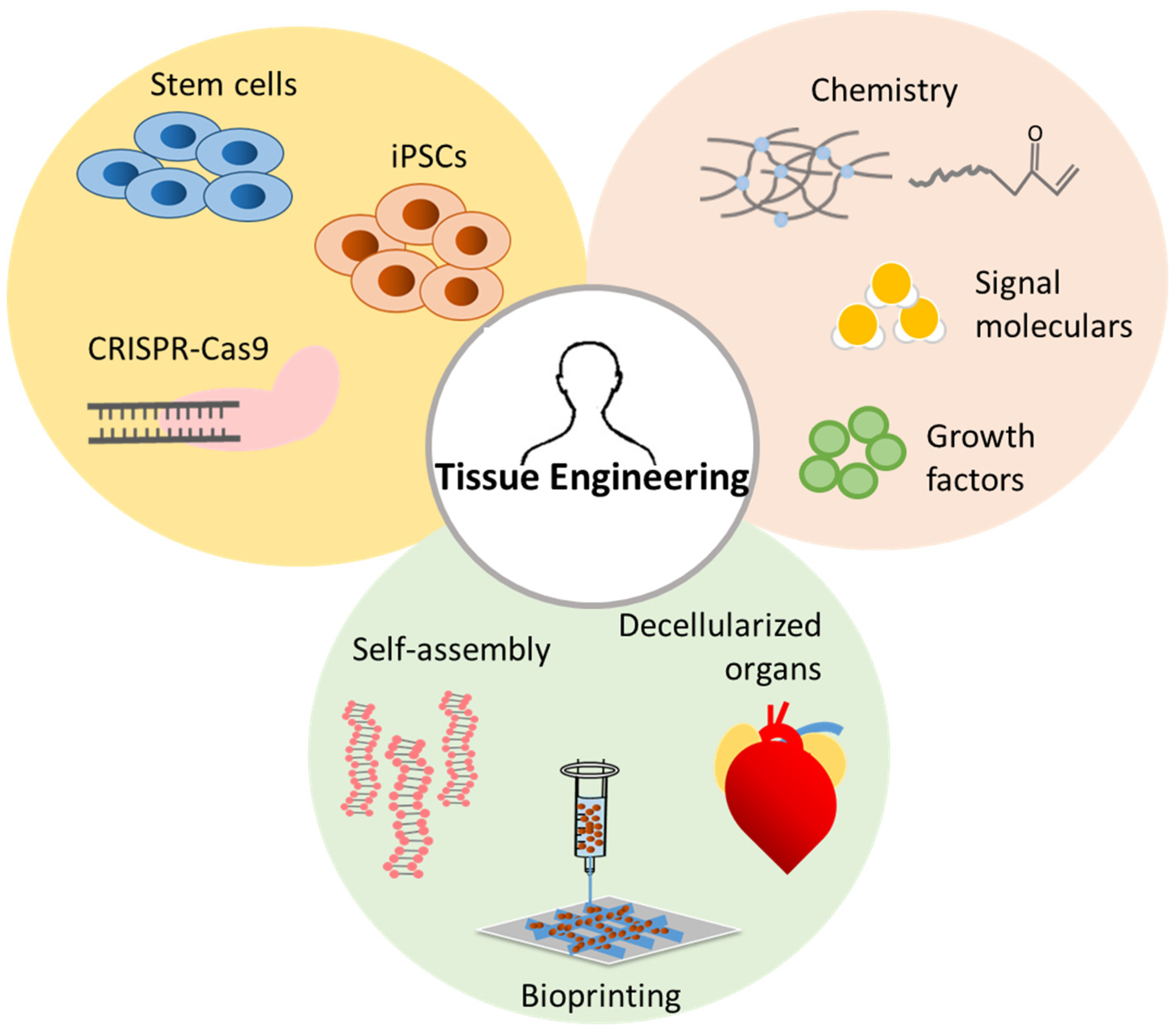
Successful periodontal regeneration is based on verifiable cementogenesis on the root surface, oblique insertion of periodontal ligament fibers and formation of new and vital supporting bone. 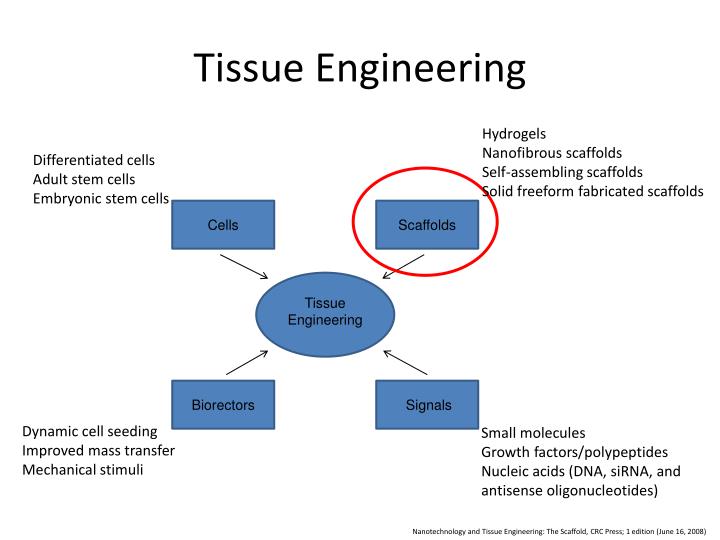
Periodontal tissue engineering involves a multi-disciplinary approach towards the regeneration of periodontal ligament, cementum and alveolar bone surrounding teeth, whereas bone regeneration specifically applies to ridge reconstruction in preparation for future implant placement, sinus floor augmentation and regeneration of peri-implant osseous defects.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
